At the end of her last blog post, Laura briefly touched upon how as well as working on the stigma surrounding mental health, a lot also needs to be done within Minority Ethnic communities. Having recently attended another talk at King’s College London: Diversity & Psychiatry: Old Battles and New Findings, she’ll now go more in-depth on the ethnic inequalities in mental health and how this issue is being tackled.
Mental health problems can affect anyone, no matter their race, gender, (dis)ability or sexual orientation. Yet there are substantial disparities in mental health treatment of individuals in minority groups, despite recent research showing Black, Asian and Minority Ethnic (BAME) groups are at a higher risk of developing a mental illness.
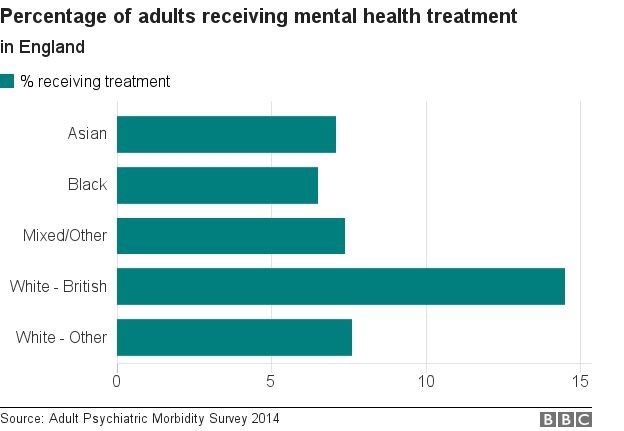
Figure taken from a BBC article on the topic
Lots of factors play into this ethnic inequality in the accessibility, experiences and outcomes of mental health care, both from within BAME communities and through service provision processes. Within the BAME communities, there is a reluctance to discuss psychological distress and acknowledge mental health problems, resulting in vulnerable people being too apprehensive or ashamed to seek help. Then there is a communication breakdown between service users and providers. The lack of sensitivity to cultural needs and discrimination towards patients from ethnic minorities, when it occurs, can result in poorer outcomes of treatment and the disengagement from mainstream mental health services. This can then often lead onto social exclusion and a deterioration in mental health.
There are already initiatives in place that aim to reduce the impact of these barriers preventing BAME communities from accessing high quality, culturally appropriate mental health support. For example, the Joint Commissioning Panel for Mental Health have a guide exclusively tailored to give practical advice on how commissioners can help adapt their services and work to eliminate racial discrimination. Work is also being done to raise awareness of this issue: in the US, the American Psychological Association (APA) launched the Diversity Mental Health Month in July 2014 as a way of educating psychiatrists and the public of the need of cultural competency in both clinical practice and research.
However, despite targeted programmes like these, initiatives aren’t always sustained and ethnic inequalities still remain entrenched within mental health services as shown by the results of the Count Me In census which found that little to no progress was made in reducing ethnic disparities in care. Therefore, more engagement with BAME communities is essential to develop services that are culturally sensitive to their needs and have a long-lasting impact, as are more anti-stigma campaigns that are tailored to the unique barriers they face.
It’s important to tackle this issue because until the mental health inequalities that minority ethnic groups face are counteracted, their communities will continue to miss out on mental health support. We can’t promote mental health awareness and the improvement of services, to be applied only to one group of people. Everyone deserves good quality mental health care.


