
Union for International Cancer Control (UICC), International Agency for Research on Cancer (IARC), and African Cancer Registry Network (AFCRN)

In April 2022, the UICC (in collaboration with the IARC and AFCRN) released an in-depth report detailing the current situation regarding cervical cancer across Africa, including the action required to achieve cervical cancer elimination as per the WHO guidelines.
The following video introduces the report’s content, main themes and recommendations.
Cervical Cancer Elimination in Africa: where are we now and where do we need to be? An introduction/summary
Presented by Sonali Johnson: Head of Knowledge, Advocacy and Policy, UICC
Read a text summary of the video here
We compiled case studies for Zimbabwe, Rwanda and Sudan to look at the current picture of cervical screening and related barriers, to understand the hurdles to overcome in order to achieve cervical cancer elimination as per the WHO guidelines.
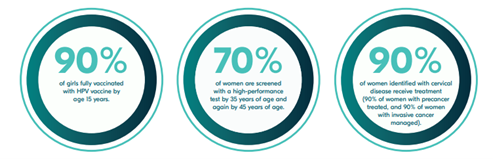
Case Studies:
ZIMBABWE
Cervical cancer is the most common cancer in Zimbabwe, and the leading cause of cancer-related deaths in the country.
The country has a history of economic crises, mainly due to a series of poor political decisions that impeded the country’s economic ascendance.
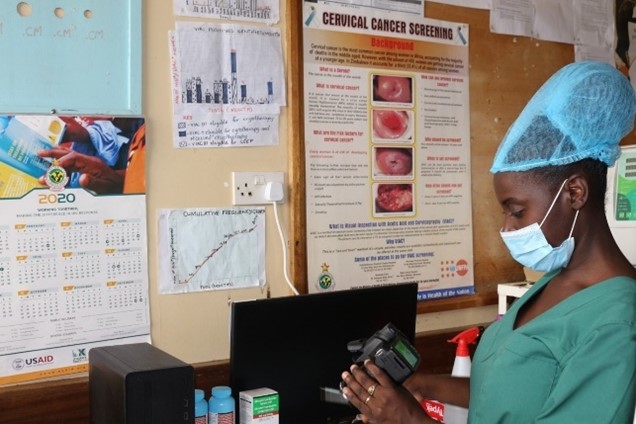
Cancer Screening and Screening Access
Cancer screening programmes are very limited in Zimbabwe. Cervical screening is only available in selected public health facilities, with private health facilities complementing these. Travel constraints and financial barriers significantly impact accessibility for the poor and rural populations.
HPV Vaccination
HPV vaccination was introduced into Zimbabwe’s routine immunisation programme in 2018.
Healthcare Provision
The main provider of healthcare services in Zimbabwe is its national public health system. This is complemented by Mission hospitals and NGO healthcare provision.
There is a limited availability of trained cervical screening providers and resources across Zimbabwe. Currently, only 9.4% of women will be screened in their lifetime in urban areas, and only 5% in rural areas.
Stigma
Cervical cancer carries significant stigma across African nations:
- The sexually transmitted nature of HPV brings shame to a diagnosis of cervical cancer.
- The strong association of cervical cancer with pre-existing HIV infection adds further stigma (HIV-positive women are 6 times more likely to develop cervical cancer compared with women without HIV). Rates of HIV in adults in Zimbabwe are 14.1%.
This stigma directly impacts screening attendance.
Transport
In rural Zimbabwe, distances from villages to health facilities remain long, with unaffordable transport costs. A 2-hour walk to the nearest hospital, to access screening services, is common. In some cases, walking distances of over 5 hours are necessary.

RWANDA
Cervical cancer is the second most common cancer in Rwanda. It is the most common cancer among Rwandan females.
However, Rwanda is on track to eliminating cervical cancer as one of the first countries globally.
Following Rwanda’s civil war and genocide of 1994, the country has committed itself to recovery and restoration. Alongside rapid socio-economic development, Rwanda has introduced a universal health care system driven by community-based health insurance. This has lowered medical costs and enabled healthcare access for even the poorest in Rwanda.
Cancer Screening and Screening Access

Rwanda has begun introducing its national-level cervical cancer screening programme in recent years. To date, around half of Rwandan health facilities have trained healthcare providers and women’s cancer clinics in place.
There is a significant commitment to cervical cancer awareness and education in Rwanda. Voluntary Community Health Workers travel from household to household in villages, sharing vital information and encouraging screening attendance.
HPV Vaccination
Rwanda was the first African country to introduce a national HPV vaccination programme, in 2011. All 12-year-old girls in school are now offered HPV vaccination. The programme has consistently achieved over 90% coverage.

Healthcare Provision
Over 80% of Rwanda’s population have free access to health services, through the country’s community-based health insurance programme.
Rwandan healthcare is delivered mainly through public hospitals, with some emerging private healthcare provision. Health facilities are comprised of:
– ‘Health posts’ and health centres, as primary care
– District hospitals and referral hospitals, as secondary care
– University teaching hospitals, as tertiary care
There are only 1.18 doctors per 10,000 people in Rwanda. (By contrast, the UK has 30.04 doctors per 10,000 people). Rwanda’s community health workers help to fill this health service delivery gap.
Stigma
To combat social stigma surrounding HPV and cervical cancer, the Rwandan government launched a large-scale national awareness campaign. This was prior to introduction of HPV vaccination across the country.
Information was delivered through community leaders, churches, village elders, health workers, schools and the media.
Transport
Transport systems in Rwanda remain unaffordable and inaccessible for much of the population, in both urban and rural areas.
With increased provision of primary healthcare across Rwanda, the average walking time to the nearest health facility has fallen to 47 minutes. The Rwandan government intends to reduce this further, to under 25 minutes by 2024.
SUDAN
Cervical cancer is the leading cause of death in women in Sudan.
Sudan has historically received much less international funding and NGO support than other African nations. This is in part due to decades of severe and prolonged political and security challenges. The country also struggles due to harsh climate conditions, a lack of natural resources and geographic isolation.

Cancer Screening and Screening Access
There are no coordinated screening programmes in Sudan, and therefore low levels of screening among Sudanese women have been reported.
With a low government health budget, screening access depends on high out-of-pocket expenditure for individuals and households. This creates obvious income-based health inequities.
HPV Vaccination
There is no current programme in Sudan for HPV vaccination.
Healthcare Provision
Sudan has a fragile health system, with only 4.57% of annual GDP (Gross Domestic Product) spent on its health system. (By contrast, the UK spends 10.15% of its annual GDP on healthcare).
Sudan has only 2.62 doctors per 10,000 people, meaning that hospitals and health services are routinely overwhelmed. (By contrast, the UK has 30.04 doctors per 10,000 people).
Additionally, there are significant regional inequalities in the distribution of healthcare services across Sudan. Most hospitals are located in urban regions, with two thirds of Sudan’s doctors working in the capital.

Credit: Dohnálek / Wikimedia Commons
Stigma
Sudan has a stigma surrounding cervical cancer, owing to the sexually transmitted nature of HPV.
Stigma due to HIV association also exists, although HIV prevalence across Sudan’s population (aged 15-49) is low, at 0.2%.
Transport
The majority of specialist health centres in Sudan are located in cities. Average travel times across Sudan, via motorised transport, are well over 5 hours.
Rural Sudan has long distances from villages to health facilities, and an unaffordability of transport costs. Where motorised transport is not available, journey times to cities are commonly a full 24 hours by foot.
The views expressed are those of the author. Posting of the blog does not signify that the Cancer Prevention Group endorse those views or opinions.

Leave a Reply