
Amanda Dibden is a statistician at Queen Mary University of London. Here she highlights the main results from her recently published worldwide review and meta-analysis of studies measuring the effect of mammography screening.
Screening for breast cancer by mammography has been in existence for over 30 years in many countries across the world. Screening aims to reduce breast cancer mortality. Given recent advances in treatment and technology, including the use of hormone therapies such as Tamoxifen and Herceptin, and moving from film to digital mammography to screen, we felt it was time to ask whether screening is still effective. We found that among those invited to screening, the risk of dying from breast cancer was reduced by 22% and among those who actually attend screening, this risk is reduced by 33%, which suggests that screening is very much a worthwhile endeavour.
Breast cancer in context
Breast cancer is an important health concern. It is the most common female cancer in the UK with around 150 women being diagnosed each day. One method used to reduce deaths from breast cancer is routine screening, the purpose of which is to diagnose cancer at an early stage when treatment is more likely to work. Almost all women diagnosed with cancer at stage one (early stage), survive for a least five years compared with about a quarter in those diagnosed at stage four (late stage), with survival having doubled over the past 40 years. This highlights the need to diagnose cancer as early as possible. Population-wide screening programmes aim to do just this by inviting women to attend regular mammography screens. In the UK, women aged 50–70 are invited every three years. However, there have been questions as to whether screening does more harm than good, and whether screening every woman aged 50–70 is cost-effective. Perhaps screening should be based on each woman’s individual risk? With these questions in mind, we wanted to assess the latest evidence to ascertain whether screening is achieving its aim of reducing the number of deaths from breast cancer.
Estimating the effectiveness of breast screening is not that simple
Assessment of the effect of screening on breast cancer mortality can be complicated by deaths from breast cancer in the screening epoch from cancers diagnosed before screening started. This biases results against screening. One can avoid this bias by analysis of rates of death by date of diagnosis.
Another complication is self-selection bias. Women who choose to attend screening may have a lower risk of dying from breast cancer than those who choose not to attend, possibly due to attenders being more health-conscious and having better health generally. A study carried out in Sweden estimated that women who choose not to attend screening have a 17% higher risk of dying from breast cancer than the general population. It is therefore important to take this bias into account as part of the statistical analysis.
Finally, the impact of screening differs if you measure the effect of being invited for screening or the effect of actually being screened. We combined the results from numerous studies to give these two different measures to assess whether screening works. The effect of being invited for screening compares women in an invited group with women who haven’t been invited. The invited group will include women who attended their invitation to screening and women who did not attend. This, therefore, measures the effect of screening in practice, where not all women will comply with their screening invitation. This measure gives a conservative estimate of the effect of screening. The other measure is the effect of actually being screened and compares women who attended their screening invitation with women who were invited but chose not to attend. Using this measure of effectiveness is complicated by self-selection bias.
What is the effectiveness of mammographic screening?
Our review brought together the results of 27 independent studies that estimated the effect of mammography screening on such incidence-based breast cancer mortality. The review included studies of screening on mortality from 11 countries, three of which were outside Europe. Screening programmes across the world differ in terms of the age at which women are invited to screening and the screening interval. However, most programmes included the age group 50–69 with a biennial screening interval.
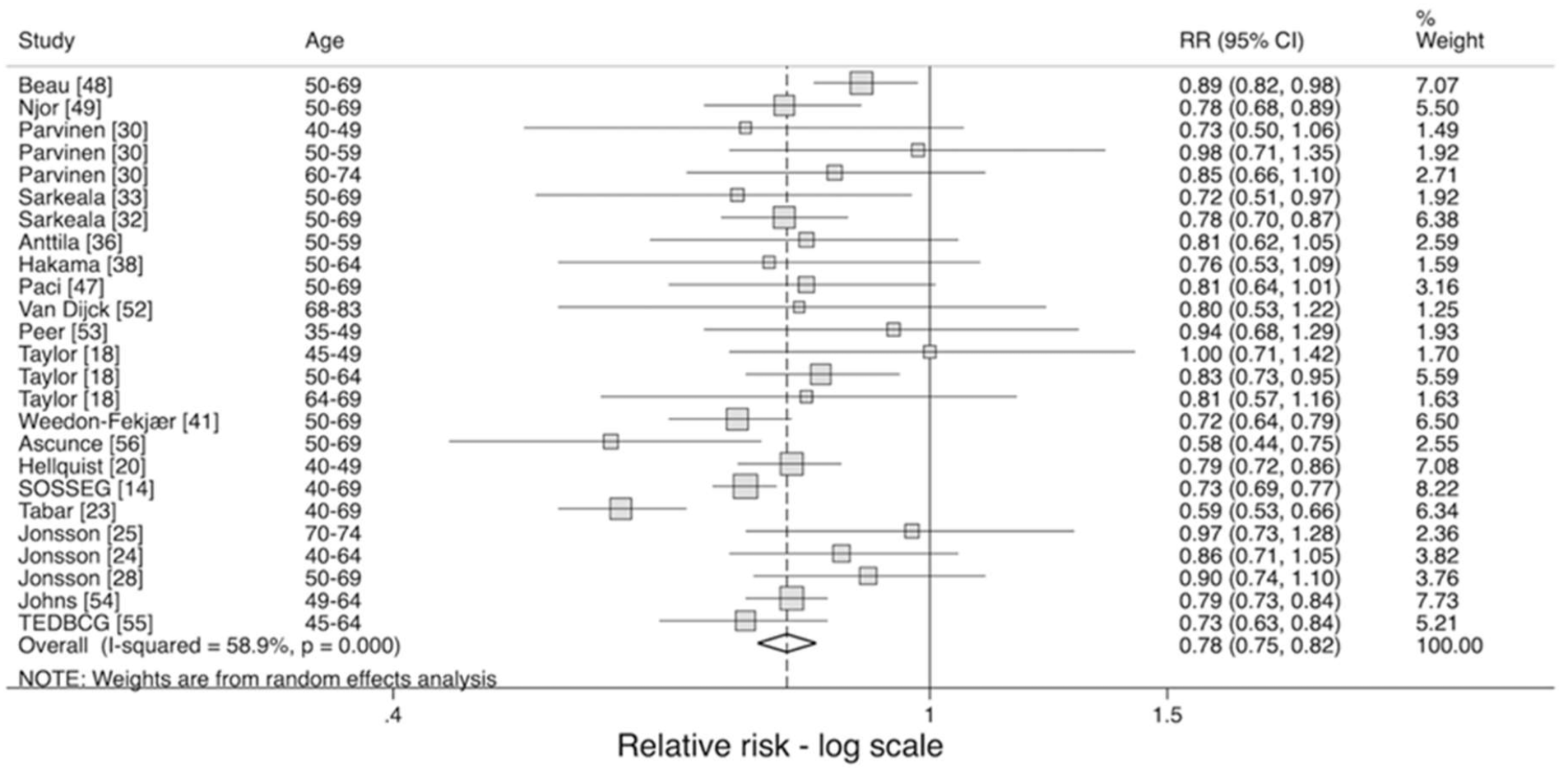
From the 27 studies included in the review, 21 studies estimated the effect of being invited to screening and we estimated that among women invited for screening the chance of dying from breast cancer is reduced by 22%. This result is in line with the earlier, formal trials into the effect of screening and suggests that having population-wide screening programmes is still worthwhile.
14 studies estimated the effect of attending mammography screening invitations. When combining the results of these studies, we found that, after correcting for self-selection bias, the risk of dying of breast cancer was 33% lower in women who accepted their screening invitation compared to those who chose not to attend. This result firmly supports the fact that attending your screening invitation is important and does reduce the chance of dying from breast cancer.
One thing that differed between the studies included in this review was the percentage of women who attended screening, the participation rate. The lowest was 44% and the highest was 92%. A screening programme is only effective at reducing deaths from breast cancer if women attend. Women should be given all the relevant information so that they can make the decision as to whether mammography screening is something they wish to participate in, both the positive and negative aspects of screening. This study did not look at any of the negative aspects of screening, which is a target for future work. The aim was to answer one question: does mammography screening reduce the risk of dying from breast cancer? and reviewing the current evidence suggests that the answer is yes it does!
The views expressed are those of the author. Posting of the blog does not signify that the Cancer Prevention Group endorse those views or opinions.

Great share! Totally agree with you. Early detection of breast cancer through mammography screening leads to numerous treatment options as compared to late detection. Moreover, as the treatment starts early, the chances of survival also increase. Appreciate your information & Good Luck for the upcoming update. Thanks.